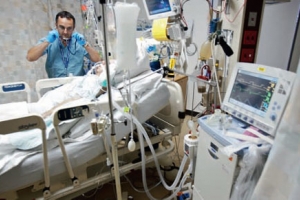
Most of humanity is now under some degree of social quarantine measures as the death toll from COVID-19 rises. As social distancing measures continue, many of you may be wondering why we don’t yet have a treatment for COVID-19. Today I’ll explain why treating viral diseases is so challenging and why some drugs may help but are not likely to offer a single game changing solution.
Facts about viruses
COVID-19 disease is caused by a virus named SARS-CoV-2. A virus is one of the simplest known microscopic organisms, usually made up of some genetic material surrounded by a protein shell. Unlike animals or bacteria, viruses lack more complex systems and need a host in which to survive and reproduce. Viruses cause diseases by invading the host’s own cells, where they hijack the host cell’s machinery to create more copies of themselves. Viral infections, including COVID-19 can also cause serious illness or death by triggering a massive inflammatory response in the body that can shut down organ systems, like the heart and lungs.
How do you treat a viral infection?
Unlike antibiotics which we can use to treat many bacterial infections, there is no available treatment that can destroy a virus once it has infected a host. The anti-viral medications that we already have at our disposal usually work by interfering with a virus’s ability to reproduce. Even if we found a way to treat COVID-19, most anti-viral medications only reduce the severity of symptoms or shorten the length of the illness. Suppressing the virus gives the body’s immune system more time and a better chance to fight off the infection. Most of the time, treatment for viral infections is limited to what we call supportive measures; a common cold or mild flu will get better with rest and fluids, whereas someone with a severe COVID respiratory infection may need ventilator support in an ICU.
Why is COVID-19 so challenging to treat?
COVID-19 is a novel disease, meaning that it is new to the world, so no one in the population has pre-existing protective immunity. COVID-19 has shown unique disease patterns that don’t fit with existing medical treatment protocols. When faced with such an urgent and deadly crisis, it’s human nature to be hopeful for a wonder drug that can end the suffering once and for all. However, it’s not that simple.
Clinical Trials
Determining whether medications are safe and effective typically involves a clinical trial where patients are enrolled in a carefully designed study where benefits and side effects of the medication are compared with a control group. Results are then subjected to rigorous statistical analysis to determine if they are actually significant. Some medical providers in hospitals caring for desperately ill COVID patients have been trying different potential therapies under what is called “compassionate use” circumstances – with the thought that a treatment that may provide even a remote chance of improvement is still better than death. If a patient is fortunate enough to recover with one of these treatments, there is no way to tell if it was because of the treatment or not, without comparison to other data in a controlled trial. As time goes on, more of these untested therapies are being used within clinical trials, but early results are still not conclusive.
Remdesivir
More and more data is being released from trials using intravenous (IV) remdesivir. It is an anti-viral medication previously developed to treat other viral infections including Ebola. Today, preliminary unreviewed results from a large placebo controlled trial were released, suggesting that giving IV remdesivir to extremely ill hospitalized patients reduced their length of hospital stay by 4 days but may not statistically reduce their chance of dying.
Additional remdesivir trials are ongoing, but so far results are mixed. Data from a trial in China indicated that remdesivir did not improve patients' conditions or reduce the presence of the virus. Other trials in the US show promise but have been criticized for poor data quality or lack of controls.
Hydroxychloroquine
Hydroxychloroquine (brand name Plaquenil®) is a medication often used to treat autoimmune diseases such as lupus. Along with its cousin chloroquine, it can also be used to treat malaria. Early in the pandemic, preliminary results from small studies in France and China suggested that a combination of hydroxychloroquine and the antibiotic azithromycin could be effective to treat COVID-19. The president and others promoted it as a potential game changer. Since then, data from these early studies has been shown to be faulty and inconclusive. Follow-up studies in France and China did not show any benefits from the treatment. Another study in Brazil was stopped after 6 days when patients receiving a higher dose of hydroxychloroquine started dying at a higher rate from irregular heart rhythms. A recent study of 368 patients at VA medical centers "found no evidence that use of hydroxychloroquine, either with or without azithromycin, reduced the risk of mechanical ventilation in patients hospitalized with Covid-19," its authors said.
Convalescent plasma
A promising therapy is the use of plasma from individuals who have had COVID-19 disease and recovered. Plasma is a straw colored fluid that is left over from blood that has had all of the red and white blood cells removed. Plasma from someone who has already had COVID-19 contains antibodies which can neutralize the virus when transfused into someone who is sick and hasn’t yet made antibodies. The main limiting factors are finding blood type compatible donors and knowing who may have recovered and have antibodies without more widespread testing available. A trial at Columbia University has just been approved by the FDA to further study the use of convalescent plasma.
Physical agents
It is well known that viruses, like any germs can be killed on surfaces or in the environment with high heat, intense ultraviolet light or strong chemicals or detergents. To be very clear, all of these agents have no benefit and are extremely dangerous or lethal if used on or inside the human body.
What the experts say
As of last week, an expert panel of the Infectious Diseases Society of America (IDSA) concluded that “There is currently insufficient evidence to recommend any particular medication for treatment of COVID-19”.
The U.S. NIH have published official treatment guidelines developed by a panel of federal agencies and professional societies. Their conclusion: “To date, no drugs have been proven to be safe and effective (or approved) to treat COVID-19. Currently, the use of any treatment drugs should be limited to patients enrolled in a clinical trial”.
The Bottom Line
Hundreds of treatment protocols are being tested around the world to try and find a spot of hope to brighten the dark specter of the COVID-19 pandemic. Preliminary data suggests that at least one medication may offer mild improvement for some patients. Potential breakthroughs will continue to be reported but must be embraced with caution. Experience with past viral pandemics like SARS, Ebola and Zika reminds us of the elusiveness of a magic bullet. We still need more data, including from proper clinical trials, which are ongoing.
Right now, the most effective tools we have to combat this epidemic remain the social distancing measures which we do know limit the spread of the disease. Only time will tell how and when the world will truly get on top of this pandemic. An effective, widely available vaccine would help to accelerate the world’s population towards herd immunity where the virus may run out of susceptible hosts to infect. This could be the game changer we are looking for, but is many months away, at best. We don’t yet know whether COVID-19 will show a seasonal pattern like the flu, or if it will mutate to be either more or less dangerous.
In the meantime, stay safe and look out for each other. Trust science and believe in humanity’s resilience to overcome catastrophe.